ASPROSIN AS A PREDICTOR OF INSULIN RESISTANCE IN NEWLY DIAGNOSED PREDIABETICS IN ASSOCIATION WITH GLYCEMIC INDICES.
Abstract
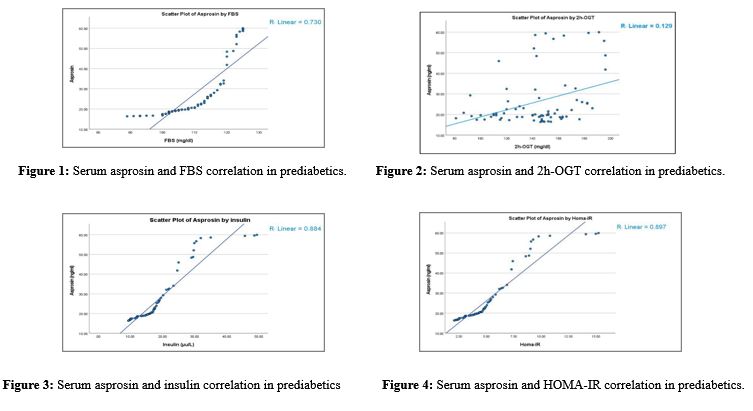
Prediabetes is a critical and sensitive stage between normal glucose levels and developing type 2 diabetes mellitus (T2DM), in which a good control can delay T2DM progression as it is closely linked to insulin resistance. The recent discovered adipokine secreted by adipose tissues, asprosin, influence glucose production and insulin sensitivity, making it a potential biomarker for insulin resistance and diabetes risk. The aim of the current study is to compare the evaluated serum asprosin levels among prediabetics and apparently healthy individuals and examine their association with glycemic indices. This case-control study was done at Duhok City, Kurdistan Region, Iraq, from October 2024 to January 2025. A total of 150 samples were collected, 75 were newly diagnosed prediabetics and 75 were apparently healthy for the control group. HbA1c%, blood sugar, insulin, and asprosin were all evaluated. Serum asprosin levels were higher in prediabetics (26.19 ± 1.49 ng/mL) compared to the control group (17.63 ± 0.51 ng/mL, p < 0.001). Within the prediabetic group, asprosin showed no significant variation across demographic or anthropometric variables, but it was significantly elevated in those with glucose levels between 140–199 mg/dL (21.95±1.25 ng/mL, p = 0.011). Moreover, asprosin was significantly higher in individuals with higher glucose levels, and strongly positively correlated with FBS, insulin, and HOMA-IR
Full text article
References
Abdullah, B.I. & Salih, S. (2023). Lipoprotein (a) Level Among Patients with Type 2 Diabetes Mellitus and Prediabetes in Comparison with Healthy Controls. Science Journal of University of Zakho, 11(1), pp.30–36. DOI: https://doi.org/10.25271/sjuoz.2023.11.1.996
Ali, S.I., Hasan, Q.I., Ali, L.I., Khaleel, F.M. and Ali, F.I. (2025). Correlation Between Asprosin and Irisin in Iraqi Patients with Type 2 Diabetes or High Blood Pressure. Baghdad Science Journal, 22(7), pp.2246–2253. DOI: https://doi.org/10.21123/2411-7986.4991
American Diabetes Association (ADA) Professional Practice Committee (2024). Diagnosis and classification of diabetes: Standards of care in diabetes—2024. Diabetes Care, 47(Suppl. 1), pp.S20–S42. Available at: https://doi.org/10.2337/dc24-S002
American Diabetes Association (ADA) (2022). Standards of medical care in diabetes—2022 abridged for primary care providers. Clinical Diabetes, 40(1), pp.10–38. DOI: https://doi.org/10.2337/cd22-as01
Bull, F.C., Al-Ansari, S.S., Biddle, S., Borodulin, K., Buman, M.P., Cardon, G., Carty, C., Chaput, J.P., Chastin, S., Chou, R. and Dempsey, P.C. (2020). World Health Organization 2020 guidelines on physical activity and sedentary behaviour. British journal of sports medicine, 54(24), pp.1451-1462. DOI: https://doi.org/10.1136/bjsports-2020-102955
Corica, D., Aversa, T., Currò, M., Tropeano, A., Pepe, G., Alibrandi, A., Ientile, R. and Wasniewska, M. (2021). Asprosin serum levels and glucose homeostasis in children with obesity. Cytokine, 142, p.155477. DOI: https://doi.org/10.1016/j.cyto.2021.155477
Elnagar, A., El-Belbasi, H.I., Rehan, I.F. and El-Dawy, K. (2018). Asprosin: a novel biomarker of type 2 diabetes mellitus. DOI: https://doi.org/10.26873/SVR-661-2018
Ertuna, G.N., Sahiner, E.S., Yilmaz, F.M. and Ates, I. (2023). The role of irisin and asprosin level in the pathophysiology of prediabetes. Diabetes Research and Clinical Practice, 199, p.110642. DOI: https://doi.org/10.1016/j.diabres.2023.110642
Farrag, M., Ait Eldjoudi, D., González-Rodríguez, M., Cordero-Barreal, A., Ruiz-Fernandez, C., Capuozzo, M., Gonzalez-Gay, M.A., Mera, A., Lago, F., Soffar, A. and Essawy, A. (2023). Asprosin in health and disease, a new glucose sensor with central and peripheral metabolic effects. Frontiers in Endocrinology, 13, p.1101091. DOI: https://doi.org/10.3389/fendo.
2022.1101091
Garg, S.S., Kushwaha, K., Dubey, R. and Gupta, J. (2023). Association between obesity, inflammation and insulin resistance: Insights into signaling pathways and therapeutic interventions. Diabetes research and clinical practice, 200, p.110691. DOI: https://doi.org/10.1016/j.diabres.2023.110691
Gozel, N. & Kilinc, F. (2021). Investigation of plasma asprosin and saliva levels in newly diagnosed type 2 diabetes mellitus patients treated with metformin. Endokrynologia Polska, 72(1), pp.37–43. DOI: https://doi.org/10.5603/EP.a2020.0059
Hekim, M.G., Kelestemur, M.M., Bulmus, F.G., Bilgin, B., Bulut, F., Gokdere, E., Ozdede, M.R., Kelestimur, H., Canpolat, S. and Ozcan, M. (2023). Asprosin, a novel glucogenic adipokine: a potential therapeutic implication in diabetes mellitus. Archives of physiology and biochemistry, 129(5), pp.1038-1044. DOI: https://doi.org/10.1080/13813455.2021.1894178
Huang, L., Fang, Y. & Tang, L. (2021). Comparisons of different exercise interventions on glycemic control and insulin resistance in prediabetes: a network meta‑analysis. BMC Endocrine Disorders, 21, p.1–13. DOI: https://doi.org/10.1186/s12902-021-00846-y
Ibrahim, I. & Salih, S. (2022). Serum irisin in individuals with type 2 diabetes Mellitus and prediabetes in Duhok City. Journal of Life and Bio Sciences Research, 3(02), pp.59–64. DOI: https://doi.org/10.38094/jlbsr30277
Lee, S.H., Park, S.Y. & Choi, C.S. (2022). Insulin resistance: from mechanisms to therapeutic strategies. Diabetes & Metabolism Journal, 46(1), pp.15–37. DOI: https://doi.org/10.4093/dmj.2021.0280
Li, Y., Chen, G.C., Moon, J.Y., Arthur, R., Sotres-Alvarez, D., Daviglus, M.L., Pirzada, A., Mattei, J., Perreira, K.M., Rotter, J.I. and Taylor, K.D. (2024). Genetic subtypes of prediabetes, healthy lifestyle, and risk of type 2 diabetes. Diabetes, 73(7), pp.1178-1187. DOI: https://doi.org/10.2337/db23-0699
Long, W., Xie, X., Du, C., Zhao, Y., Zhang, C., Zhan, D., Li, Z., Ning, Q. and Luo, X. (2019). Decreased circulating levels of asprosin in obese children. Hormone research in paediatrics, 91(4), pp.271-277. DOI: https://doi.org/10.1159/000500523
Magkos, F., Lee, M.H., Lim, M., Cook, A.R., Chhay, V., Loh, T.P., Chia, K.S., Baig, S., Ang, I.Y.H., Tay, J.Y. and Khoo, C.M. (2022). Dynamic assessment of insulin secretion and insulin resistance in Asians with prediabetes. Metabolism, 128, p.154957. DOI: https://doi.org/10.1016/j.metabol.2021.154957
Małkowska, P. (2024). Positive Effects of Physical Activity on Insulin Signaling. Current Issues in Molecular Biology, 46(6), pp.5467–5487. DOI: https://doi.org/10.3390/cimb46060327
Maylem, E.R.S., Spicer, L.J., Batalha, I. and Schutz, L.F. (2021). Discovery of a possible role of asprosin in ovarian follicular function. Journal of molecular endocrinology, 66(1), pp.35-44. DOI: https://doi.org/10.1530/JME-20-0218
Mirr, M., Braszak-Cymerman, A., Ludziejewska, A., Kręgielska-Narożna, M., Bogdański, P., Bryl, W. and Owecki, M. (2023). Serum asprosin correlates with indirect insulin resistance indices. Biomedicines, 11(6), p.1568. DOI: https://doi.org/10.3390/biomedicines11061568
Mishra, I. & Chopra, A.R. (2022). Overexpression and ELISA‑based detection of asprosin in cultured cells and mice. STAR Protocols, 3(4), p.101762. DOI: https://doi.org/10.3390/biomedicines11061568
Othman, P. K., & Kakey , I. S. (2023). EVALUATION OF THYROID FUNCTION MARKERS IN TYPE 2 DIABETIC PATIENTS IN RELATION TO INSULIN RESISTANCE. Science Journal of University of Zakho, 11(2), 237–243. https://doi.org/10.25271/sjuoz.2023.11.2.1063
Rathod, L., Khan, S., Shubham, S., Bisne, N., Singh, S., Kumar, M., Tiwari, R. and Sarma, D.K. (2024). A comparative evaluation of point-of-care and laboratory HbA1c testing in diabetes care: an Indian perspective. Cureus, 16(9). DOI: https://doi.org/10.7759/cureus.69956
Salih, S. (2024). Association of Lipoprotein and Apolipoprotein Ratios With Glycemic Levels in Individuals With Prediabetes: A Case‑Control Study. Cureus, 16(6). DOI: https://doi.org/10.7759/cureus.63500
Sathiya, V. & Kumar, V.R. (2024). Harmonised Methods for Detection of Insulin Immunogenicity. International Journal of Pharmaceutical Investigation, 14(2). DOI: https://doi.org/10.5530/ijpi.14.2.38
Shabir, K., Brown, J.E., Afzal, I., Gharanei, S., Weickert, M.O. & Barber, T.M. (2021). Asprosin, a novel pleiotropic adipokine implicated in fasting and obesity-related cardio‑metabolic disease: comprehensive review of preclinical and clinical evidence. Cytokine & Growth Factor Reviews, 60, pp.120–132. DOI: https://doi.org/10.1016/j.cytogfr.2021.05.002
Sulaiman, D.M. (2021). Evaluation of serum asprosin levels in women with metabolic syndrome in Duhok City – Kurdistan Region, Iraq. International Journal of Research in Medical Sciences, 9(7), pp.1978–1983. DOI: https://doi.org/10.18203/2320-6012.ijrms20213067
Suleiman, R.R., Fathi Ali, A., Salih, S.F. & Abdullah, B.I. (2023). Prevalence of Insulin Resistance Among Apparently Healthy Medical Students of College of Health and Medical Technology–Shekhan. History of Medicine, 9(1), pp.918–925. DOI: https://doi.org/10.17720/2409-5834.v9.1.2023.105
Suleiman, R.R., Salih, S.F., Abdullah, B.I., Ibrahim, I.H. & Saeed, Z.A. (2023). Triglyceride Glucose Index, its Modified Indices, and Triglyceride HDL‑C Ratio as Predictor Markers of Insulin Resistance in Prediabetic Individuals. Medical Journal of Babylon, 20(2), pp.268–273. DOI: DOI: https://doi.org/10.4103/MJBL.MJBL_269_22
Summers, K.M., Bush, S.J., Davis, M.R., Hume, D.A., Keshvari, S. and West, J.A. (2023). Fibrillin-1 and asprosin, novel players in metabolic syndrome. Molecular Genetics and Metabolism, 138(1), p.106979. DOI: https://doi.org/10.1016/j.ymgme.2022.106979
Tylutka, A., Walas, Ł. & Zembron‑Lacny, A. (2024). Level of IL‑6, TNF, and IL‑1β and age-related diseases: a systematic review and meta‑analysis. Frontiers in Immunology, 15, p.1330386. DOI: https://doi.org/10.3389/fimmu.2024.1330386
Wang, M., Yin, C., Wang, L., Liu, Y., Li, H., Li, M., Yi, X. and Xiao, Y. (2020). Serum asprosin concentrations are increased and associated with insulin resistance in children with obesity. Annals of nutrition and metabolism, 75(4), pp.205-212. DOI: https://doi.org/10.1159/000503808
Wang, Y., Qu, H., Xiong, X., Qiu, Y., Liao, Y., Chen, Y., Zheng, Y. and Zheng, H. (2018). Plasma asprosin concentrations are increased in individuals with glucose dysregulation and correlated with insulin resistance and first‐phase insulin secretion. Mediators of inflammation, 2018(1), p.9471583. DOI: https://doi.org/10.1155/2018/9471583
World Health Organization (WHO) (2024). Obesity and overweight. Available at: https://www.who.int/news-room/fact-sheets/detail/obesity-and-overweight
Zhang, Y., Zhang, Y., Yang, B., Li, S. and Jia, R. (2024). Circulating levels of asprosin in children with obesity: a systematic review and meta-analysis. BMC Endocrine Disorders, 24(1), p.36. DOI: https://doi.org/10.1186/s12902-024-01565-w
Zhang, Z., Zhu, L., Wang, Z., Hua, N., Hu, S. & Chen, Y. (2023). Can the new adipokine asprosin be a metabolic troublemaker for cardiovascular diseases? A state‑of‑the‑art review. Progress in Lipid Research, 91, p.101240. DOI: https://doi.org/10.1016/j.plipres.2023.101240
Authors
Copyright (c) 2026 Huda N. Salih, and Sherwan F. Salih

This work is licensed under a Creative Commons Attribution-NonCommercial-ShareAlike 4.0 International License.
Authors who publish with this journal agree to the following terms:
- Authors retain copyright and grant the journal right of first publication with the work simultaneously licensed under a Creative Commons Attribution License [CC BY-NC-SA 4.0] that allows others to share the work with an acknowledgment of the work's authorship and initial publication in this journal.
- Authors are able to enter into separate, additional contractual arrangements for the non-exclusive distribution of the journal's published version of the work, with an acknowledgment of its initial publication in this journal.
- Authors are permitted and encouraged to post their work online.