EXPLORING THE ONCOGENIC AND TUMOR SUPPRESSIVE FUNCTIONS OF hsa-miR-125B AND hsa-miR-574 IN ACUTE LYMPHOBLASTIC LEUKEMIA
Abstract
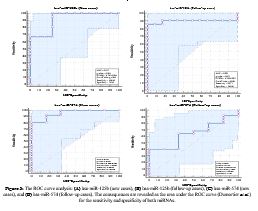
Acute lymphoblastic leukemia (ALL) is the second common type of leukemia. In leukemia, small non-coding RNAs (miRNAs) role as either tumor suppressors or oncomiRNAs. Evidence indicates an association between the dysregulation of these miRNAs and the progression and spread. An essential regulator in carcinogenesis and progression, hsa-miR-574 is up- or down-regulated by functional pathways, underlying new mechanisms. ALL prognosis and chemoresistance have both been linked to hsa-miR-125b. Quantitative real-time polymerase chain reaction was employed to analyses the expression levels of hsa-miR-125b and hsa-miR-574 in 25 ALL patients (new and follow-up cases) and 20 healthy controls. The findings indicated that the expression levels of hsa-miR-125b and hsa-miR-574 are modified in ALL, and their expression levels were markedly changed in ALL patients. The hsa-miR-125b expression level was upregulated in new cases and downregulated in follow-up cases. Conversely, hsa-miR-574 was downregulated in ALL new cases compared to controls. However, these levels increased in follow-up cases undergoing chemo-immunotherapy. The statistics derived from the ROC curve indicate that hsa-miR-125b expression in new cases had an AUC = 0.762, in follow-up cases had an AUC = 0.562, while the hsa-miR-574 expression in new cases had an AUC = 0.542 and in follow-up cases with an AUC = 0.916 were correlated with the ALL instances. The hsa-miR-125b upregulation observed in ALL suggests its potential oncogenic role. Conversely, the downregulation of hsa-miR-574 predicts a possible tumor-suppressive function, given its reduced expression. These findings highlight the significance of hsa-miR-125b and hsa-miR-574 as key regulatory molecules in ALL progression.
Full text article
References
Almeida, R. S., Costa e Silva, M., Coutinho, L. L., Garcia Gomes, R., Pedrosa, F., Massaro, J. D., Donadi, E. A., & Lucena‐Silva, N. (2019). MicroRNA expression profiles discriminate childhood T‐from B‐acute lymphoblastic leukemia. Hematological oncology, 37(1), 103-112. https://doi.org/10.1002/hon.2567
Alsuwaidi, L., Hachim, M., & Senok, A. (2021). Novel markers in pediatric acute lymphoid leukemia: the role of ADAM6 in B cell leukemia. Frontiers in Cell and Developmental Biology, 9, 706129. https://doi.org/10.3389/fcell.2021.706129
Anelli, L., Zagaria, A., Specchia, G., Musto, P., & Albano, F. (2021). Dysregulation of miRNA in Leukemia: Exploiting miRNA Expression Profiles as Biomarkers. International journal of molecular sciences, 22(13), 7156. https://www.mdpi.com/1422-0067/22/13/7156
Baradaran, B., Shahbazi, R., & Khordadmehr, M. (2019). Dysregulation of key microRNAs in pancreatic cancer development. Biomed Pharmacother, 109, 1008-1015. https://doi.org/10.1016/j.biopha.2018.10.177
Bousquet, M., Harris, M. H., Zhou, B., & Lodish, H. F. (2010). MicroRNA miR-125b causes leukemia. Proc Natl Acad Sci U S A, 107(50), 21558-21563. https://doi.org/10.1073/pnas.1016611107
Colorado-Yohar, S. M., Castillo-González, A. C., Sánchez-Meca, J., Rubio-Aparicio, M., Sánchez-Rodríguez, D., Salamanca-Fernández, E., Ardanaz, E., Amiano, P., Fernández, M. F., Mendiola, J., Navarro-Mateu, F., & Chirlaque, M. D. (2021). Concentrations of bisphenol-A in adults from the general population: A systematic review and meta-analysis. Sci Total Environ, 775, 145755. https://doi.org/10.1016/j.scitotenv.2021.145755
Dawidowska, M., Jaksik, R., Drobna, M., Szarzyńska-Zawadzka, B., Kosmalska, M., Sędek, Ł., Machowska, L., Lalik, A., Lejman, M., & Ussowicz, M. (2019). Comprehensive investigation of miRNome identifies novel candidate miRNA-mRNA interactions implicated in T-cell acute lymphoblastic leukemia. Neoplasia, 21(3), 294-310. https://doi.org/10.1016/j.neo.2019.01.004
de Oliveira, J. C., Brassesco, M. S., Scrideli, C. A., Tone, L. G., & Narendran, A. (2012). MicroRNA expression and activity in pediatric acute lymphoblastic leukemia (ALL). Pediatric Blood & Cancer, 59(4), 599-604. https://doi.org/10.1002/pbc.24167
Dumortier, O., Fabris, G., Pisani, D. F., Casamento, V., Gautier, N., Hinault, C., Lebrun, P., Duranton, C., Tauc, M., Dalle, S., Kerr-Conte, J., Pattou, F., Prentki, M., & Van Obberghen, E. (2020). microRNA-375 regulates glucose metabolism-related signaling for insulin secretion. J Endocrinol, 244(1), 189-200. https://doi.org/10.1530/JOE-19-0180
Duyu, M., Durmaz, B., Gunduz, C., Vergin, C., Yilmaz Karapinar, D., Aksoylar, S., Kavakli, K., Cetingul, N., Irken, G., & Yaman, Y. (2014). Prospective evaluation of whole genome microRNA expression profiling in childhood acute lymphoblastic leukemia. BioMed research international, 2014(1), 967585. https://doi.org/10.1155/2014/967585
García‑Alcocer, G., & Becerra, E. (2020). MicroRNAs and Their Role in Acute Lymphoblastic Leukemia. In P. P. Piccaluga (Ed.), Acute Leukemias. IntechOpen. https://doi.org/10.5772/intechopen.94960
Gefen, N., Binder, V., Zaliova, M., Linka, Y., Morrow, M., Novosel, A., Edry, L., Hertzberg, L., Shomron, N., Williams, O., Trka, J., Borkhardt, A., & Izraeli, S. (2010). Hsa-mir-125b-2 is highly expressed in childhood ETV6/RUNX1 (TEL/AML1) leukemias and confers survival advantage to growth inhibitory signals independent of p53. Leukemia, 24(1), 89-96. https://doi.org/10.1038/leu.2009.208
Grobbelaar, C., & Ford, A. M. (2019). The role of MicroRNA in paediatric acute lymphoblastic leukaemia: challenges for diagnosis and therapy. Journal of Oncology, 2019(1), 8941471. https://doi.org/10.1155/2019/8941471
Hartle, J. C., Fox, M. A., & Lawrence, R. S. (2016). Probabilistic modeling of school meals for potential bisphenol A (BPA) exposure. Journal of Exposure Science & Environmental Epidemiology, 26(3), 315-323. https://doi.org/10.1038/jes.2015.58
Kyriakidis, I., Kyriakidis, K., & Tsezou, A. (2022). MicroRNAs and the Diagnosis of Childhood Acute Lymphoblastic Leukemia: Systematic Review, Meta-Analysis and Re-Analysis with Novel Small RNA-Seq Tools. Cancers, 14(16), 3976. https://doi.org/doi:10.3390/cancers14163976
Liang, C., Li, Y., Wang, L.-N., Zhang, X.-L., Luo, J.-S., Peng, C.-J., Tang, W.-Y., Huang, L.-B., Tang, Y.-L., & Luo, X.-Q. (2021). Upregulated miR-155 is associated with poor prognosis in childhood acute lymphoblastic leukemia and promotes cell proliferation targeting ZNF238. Hematology, 26(1), 16-25. https://doi.org/10.1080/16078454.2020.1860187
Liu, Z., Smith, K. R., Khong, H. T., Huang, J., Ahn, E.-Y. E., Zhou, M., & Tan, M. (2016). miR-125b regulates differentiation and metabolic reprogramming of T cell acute lymphoblastic leukemia by directly targeting A20. Oncotarget, 7(48), 78667.
Lyssenko, V., Jonsson, A., Almgren, P., Pulizzi, N., Isomaa, B., Tuomi, T., Berglund, G., Altshuler, D., Nilsson, P., & Groop, L. (2008). Clinical risk factors, DNA variants, and the development of type 2 diabetes. N Engl J Med, 359(21), 2220-2232. https://doi.org/10.1056/NEJMoa0801869
Mak, K. W. Y., He, W., Loganathan, N., & Belsham, D. D. (2023). Bisphenol A Alters the Levels of miRNAs That Directly and/or Indirectly Target Neuropeptide Y in Murine Hypothalamic Neurons. Genes, 14(9), 1773. https://doi.org/doi:10.3390/genes14091773
Mendiola-Soto, D. K., Bárcenas-López, D. A., Pérez-Amado, C. J., Cruz-Miranda, G. M., Mejía-Aranguré, J. M., Ramírez-Bello, J., Hidalgo-Miranda, A., & Jiménez-Morales, S. (2023). MiRNAs in Hematopoiesis and Acute Lymphoblastic Leukemia. International journal of molecular sciences, 24(6), 5436. https://doi.org/doi:10.3390/ijms24065436
Moqadam, F. A., Lange-Turenhout, E., Pieters, R., & Den Boer, M. L. (2012). Collaboration Between MiR-125b, MiR-100 and MiR-99a Induces Vincristine Resistance in Childhood TEL-AML1-Positive Acute Lymphoblastic Leukemia. Blood, 120(21), 1475-1475. https://doi.org/10.1182/blood.V120.21.1475.1475
Muhsin, A. A., Atrushi, A. M., & Al-Doski, A. A. (2024). THE SIGNIFICANCE OF MINIMAL RESIDUAL DISEASE IN ACUTE LYMPHOBLASTIC LEUKAEMIA: A SINGLE CENTRE STUDY. Science Journal of University of Zakho, 12(2), 144-148. https://doi.org/10.25271/sjuoz.2024.12.2.1240
Nothnick, W. B., Healy, C., & Hong, X. (2010). Steroidal regulation of uterine miRNAs is associated with modulation of the miRNA biogenesis components Exportin-5 and Dicer1. Endocrine, 37, 265-273. https://doi.org/10.1007/s12020-009-9293-9
Piatopoulou, D., Avgeris, M., Marmarinos, A., Xagorari, M., Baka, M., Doganis, D., Kossiva, L., Scorilas, A., & Gourgiotis, D. (2017). miR-125b predicts childhood acute lymphoblastic leukaemia poor response to BFM chemotherapy treatment. British Journal of Cancer, 117(6), 801-812. https://doi.org/10.1038/bjc.2017.256
Pui, C.-H., Mullighan, C. G., Evans, W. E., & Relling, M. V. (2012). Pediatric acute lymphoblastic leukemia: where are we going and how do we get there? Blood, The Journal of the American Society of Hematology, 120(6), 1165-1174. https://doi.org/10.1182/blood-2012-05-378943
Rasdi, Z., Kamaludin, R., Ab. Rahim, S., Syed Ahmad Fuad, S. B., Othman, M. H. D., Siran, R., Mohd Nor, N. S., Abdul Hamid Hasani, N., & Sheikh Abdul Kadir, S. H. (2020). The impacts of intrauterine Bisphenol A exposure on pregnancy and expression of miRNAs related to heart development and diseases in animal model. Scientific Reports, 10(1), 5882. https://doi.org/10.1038/s41598-020-62420-1
Rezg, R., El-Fazaa, S., Gharbi, N., & Mornagui, B. (2014). Bisphenol A and human chronic diseases: current evidences, possible mechanisms, and future perspectives. Environment international, 64, 83-90. https://doi.org/10.1016/j.envint.2013.12.007
Schotte, D., Pieters, R., & Den Boer, M. L. (2012). MicroRNAs in acute leukemia: from biological players to clinical contributors. Leukemia, 26(1), 1-12. https://doi.org/10.1038/leu.2011.151
So, A. Y.-L., Sookram, R., Chaudhuri, A. A., Minisandram, A., Cheng, D., Xie, C., Lim, E. L., Flores, Y. G., Jiang, S., Kim, J. T., Keown, C., Ramakrishnan, P., & Baltimore, D. (2014). Dual mechanisms by which miR-125b represses IRF4 to induce myeloid and B-cell leukemias. Blood, 124(9), 1502-1512. https://doi.org/10.1182/blood-2014-02-553842
Szczepanek, J. (2020). Role of microRNA dysregulation in childhood acute leukemias: Diagnostics, monitoring and therapeutics: A comprehensive review. World journal of clinical oncology, 11(6), 348. https://doi.org/10.5306/wjco.v11.i6.348
Tebbi, C. K. (2021). Etiology of Acute Leukemia: A Review. Cancers (Basel), 13(9). https://doi.org/10.3390/cancers13092256
Terwilliger, T., & Abdul-Hay, M. (2017). Acute lymphoblastic leukemia: a comprehensive review and 2017 update. Blood Cancer Journal, 7(6), e577-e577. https://doi.org/10.1038/bcj.2017.53
Yang, H., Zhang, J., Li, J., Zhao, F., Shen, Y., & Xing, X. (2018). Overexpression of miR-574-3p suppresses proliferation and induces apoptosis of chronic myeloid leukemia cells via targeting IL6/JAK/STAT3 pathway. Exp Ther Med, 16(5), 4296-4302. https://doi.org/10.3892/etm.2018.6700
Yang, J. Y. (2024). miR-574-5p in epigenetic regulation and Toll-like receptor signaling. Cell Communication and Signaling, 22(1), 567. https://doi.org/10.1186/s12964-024-01934-x
Authors
Copyright (c) 2026 Soran Ali Yaba, and Rebwar Muhammad Hamasalih

This work is licensed under a Creative Commons Attribution-NonCommercial-ShareAlike 4.0 International License.
Authors who publish with this journal agree to the following terms:
- Authors retain copyright and grant the journal right of first publication with the work simultaneously licensed under a Creative Commons Attribution License [CC BY-NC-SA 4.0] that allows others to share the work with an acknowledgment of the work's authorship and initial publication in this journal.
- Authors are able to enter into separate, additional contractual arrangements for the non-exclusive distribution of the journal's published version of the work, with an acknowledgment of its initial publication in this journal.
- Authors are permitted and encouraged to post their work online.